RJAH

Alice Ward at Robert Jones & Agnes Hunt Orthopaedic Hospital (RJAH)
Who do we coordinate education for?
Alice Ward is the children’s orthopaedic surgery and rehabilitation 16 bed ward at the Robert Jones & Agnes Hunt Orthopaedic Hospital (RJAH). Children and young people, between the ages of 0-17 years, are routinely admitted for planned surgery, intensive physiotherapy and rehabilitation. In-patient stays can be both short -term and long-term and the Trust serves people from both England and Wales with some patients travelling significant distances for their medical treatment

Alice Ward provides specialist advice, diagnosis and treatment for the whole spectrum of bone, joint and muscular disorders during childhood, including treatment of:
Spinal deformity & spinal injury, Cerebral Palsy, Chronic Regional Pain Syndrome (CRPS), Developmental Dysplasia of the hip, Leg Length Discrepancy, Rheumatology, Limb Deficiency & Prosthesis, Skeletal Dysplasia, Sports Injuries, Muscular dystrophy, Congenital Hip Dislocation, Foot Problems, Club Foot.
Patients are generally registered with schools across both England and Wales attending mainstream and specialist provision or Elective Home Education (EHE).


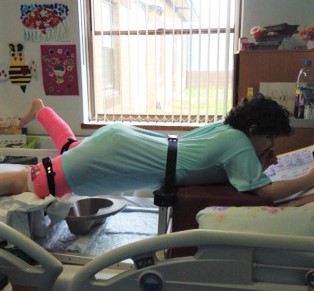
Where do we work?
Alice Ward has an open-plan classroom area suitable for both wheelchair and bed access where patients can be taught in small groups or on a 1:1 basis. There is also flexibility to teach at a patient’s bedside when this may be the most suitable option.
What do we teach?
The Hospital Educational Coordinator monitors educational provision for patients on the ward and establishes that they have an educational provider.
Teaching sessions are provided alongside inpatient nursing, physiotherapy, hydrotherapy and any other medical procedures which are required during an inpatient stay.
On admittance to the ward, an initial meeting with the patient and parent/carer enables relevant medical and educational information to be gathered. This also allows patients and carers to understand the TMBSS educational provision available on the ward. Positive relationships are very quickly formed with each patient and their families and allows for the opportunity to understand the impact that a patients’ medical condition and treatment may have upon their access to education.
Communication and liaison between the patients’ usual school setting helps to rapidly establish an accurate starting point to build flexible, personalised learning programmes. Appropriate to each patient, these can encompass the whole curriculum and not only encourage academic development but also reflect patients changing medical and mental health needs. Information regarding academic achievements, safeguarding concerns and attendance can also be communicated between schools and the Hospital Educational Coordinator. Patients’ school curriculums and the programmes of study provided by their school are our main focus for the delivery of teaching and learning. However, if these are not suitable or available, a wide variety of resources are accessible to the Hospital Educational Coordinator, allowing for any gaps in learning to be recognised whilst providing suitable challenges and opportunities for progression.
The TMBSS whole service curriculum is derived from the National Curriculum to engage patients and is often used in combination with usual school curriculums. TMBSS assessments can be used as required with support and advice from TMBSS curriculum specialists requested as needed. Our teaching provision focuses on overcoming barriers where specific medical, social, academic and mental health needs are met to access education in a positive, self-affirming manner.
How do we support our patients & promote wellbeing?
The Hospital Educational Coordinator supports school aged patients throughout their admission, including those with profound and multiple learning difficulties with a commitment to creating a nurturing, empowering learning environment. Positive relationships are quickly established with each patient and family focusing upon a holistic, collaborative multi-disciplinary team approach to their wellbeing. This not only acknowledges the challenges a patient may face, but also motivates and nurtures their self-esteem and confidence.
Patients often present with high levels of anxiety and so the Hospital Educational Coordinator is able to respond and engage appropriately with a highly flexible, bespoke approach that encourages a sense of normality and nurture. This leads to a more confident, positive outlook towards learning, supporting their challenges toward recovery and transition back to their usual home schools. For long-term patients, the arranging of online Teams meetings allows the chance to connect with their usual school setting and provides opportunities for professionals to collaborate whilst supporting the patient and their families.
For those patients needing to take exams whilst in hospital, provision can be made for a personalised approach to exam preparation. In the past, we have liaised with schools and facilitated for patients to sit both GCSE exams and Yr. 6 SATs whilst in hospital if appropriate.
The nature of our teaching provision endeavours to maintain a sense of normality for patient’s whilst in hospital, celebrating their achievements and successes, and encouraging resilience and independence.
For those patients transitioning back into school after an extended absence, the Hospital Educational Coordinator liaises closely with medical staff and the usual school setting to ensure a smooth transition which considers the challenges each patient faces.
How do we communicate, review and report?
The intent, implementation and impact of teaching sessions with patients are recorded daily alongside an electronic register. A weekly return sheet is also completed summarising the support provided by the Hospital Educational Coordinator which is shared with the TMBSS senior leadership team.
The Hospital Educational Coordinator attends daily handover meetings with nursing staff and physiotherapists on the ward to maintain ongoing, effective communication. A paediatric forum is also held on the ward each month and the Hospital Educational Coordinator also attends MDT planning meetings for paediatric spinal cord injury patients with the Midland Centre for Spinal Injuries team.
The Hospital Educational Coordinator also works closely with the Play Specialist Team and other agencies and professionals who are involved with each patient. Liaison with a patient’s usual school facilitates a bespoke curriculum which offers appropriate levels of support and challenge.
A collaborative working partnership exists between Hospital Educational Coordinators at RJAH and PRH hospitals with the sharing of good practice. Regular meetings are held and include:
- Half-termly meetings with TMBSS Line Manager & TMBSS Head of Service.
- Half-termly in person / Huddle meetings via Teams between Hospital Educational Coordinators at RJAH and PRH.
- Attendance at TMBSS Personal Development, Welfare & Behaviour Working Party.
Safeguarding
The Hospital Educational Coordinator on the ward is a trained Designated Safeguarding Lead and receives regular training updates.
Any safeguarding concerns are reported to the Designated Safeguarding Lead on Alice Ward where the safeguarding referral process is followed.
Liaison with TMBSS and safeguarding procedures are followed as appropriate.
A central electronic register (Child Protection Information Sharing, CPIS) is used on the ward which alerts staff to key information such as whether a child is subject to a child protection plan or is a looked after child.
This information is shared during handover meetings and recorded in the safeguarding section of the Patient Pathway file on admission which the Hospital Educational Coordinator can view.
Accessibility Plan
All Accessibility plans can be found on the SEND page.
